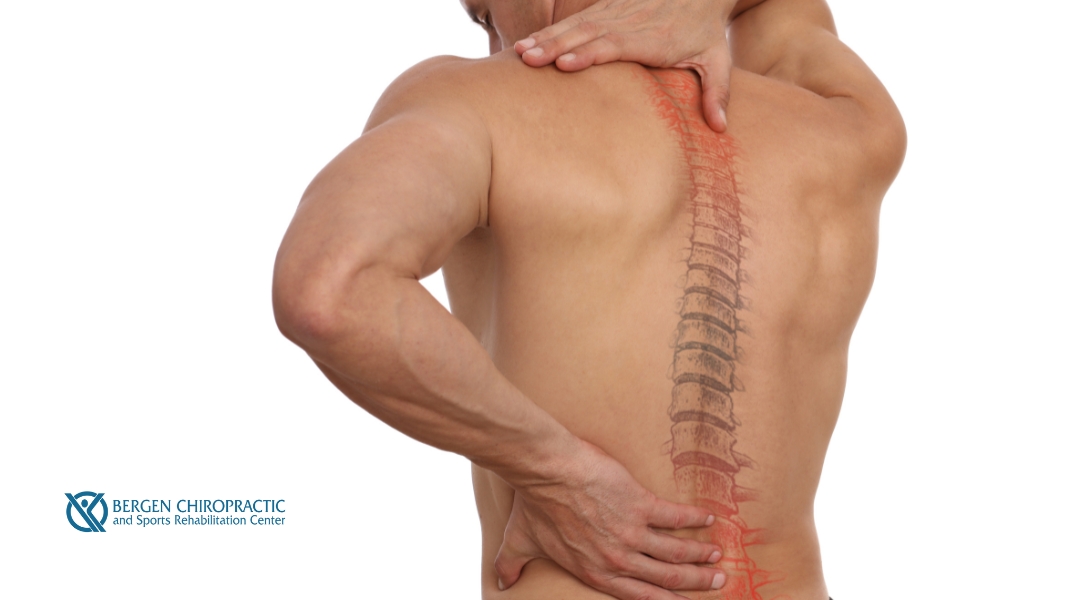
Chiropractic care eases RA joint pain, improves mobility, and complements your holistic rheumatoid arthritis treatment plan.
8 Chronic Conditions Managed by Chiropractic Care
Learn how chiropractic care safely eases hand numbness during pregnancy at Bergen Chiropractic.
Chiropractic Solutions for Pregnancy-Related Hand Numbness
Relieve pregnancy hand numbness with expert chiropractic care and gentle techniques at Bergen Chiropractic.
Aligning for Two: Chiropractic Solutions for Prenatal Joint Pain
Chiropractic care eases prenatal joint pain with safe, effective solutions for expectant mothers at Bergen Chiropractic.
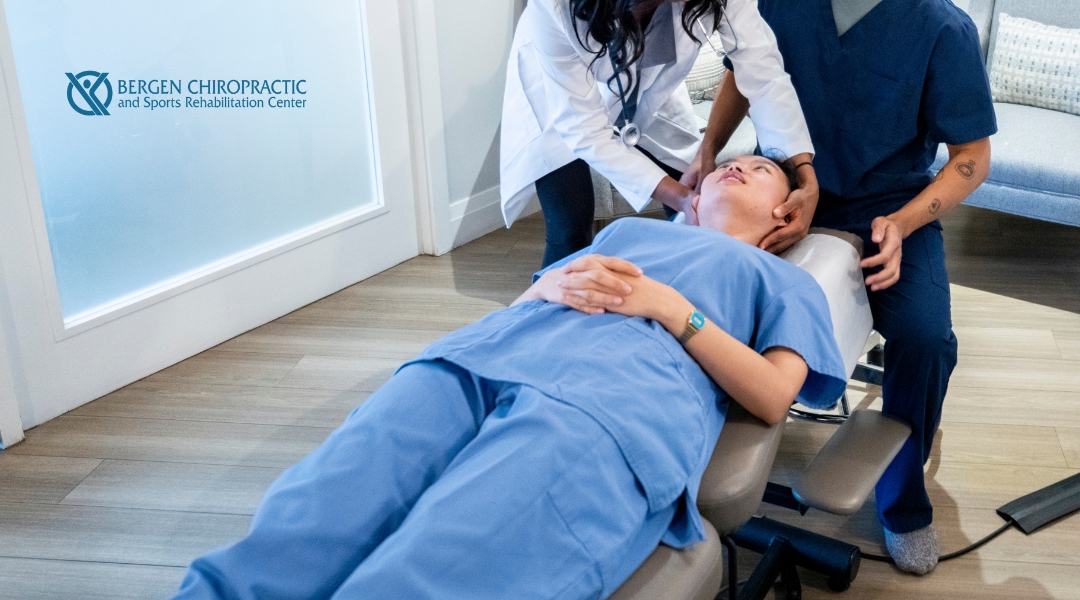
Enhancing Chiropractic Skills in Bergen County, NJ: Practitioner Training at Bergen Chiropractic
Enhance your chiropractic skills with expert training at Bergen Chiropractic in Bergen County, NJ, designed for practitioners seeking to expand their expertise.
Relieving Hip Pain in Bergen County, NJ: How a Local Chiropractor Can Help
Learn how a local chiropractor in Bergen County, NJ, can help relieve hip pain with effective, natural treatments tailored to your needs.
Chiropractic Care Helps Recover From Skiing Injuries!
Chiropractic care helps athletes recover from skiing injuries, offering pain relief and improved mobility for a smoother, faster return to the slopes.
How Chiropractic Care Supports Mothers With C-Section Scars
Chiropractic care can help mothers heal from C-section scars, easing discomfort and promoting recovery for a healthier, more comfortable postpartum experience.
Align for Adventure: Chiropractic Benefits for Outdoor Enthusiasts This Spring
Ready to enjoy the outdoors this spring? Chiropractic care for outdoor enthusiasts improves flexibility, prevents injuries, and supports better movement.
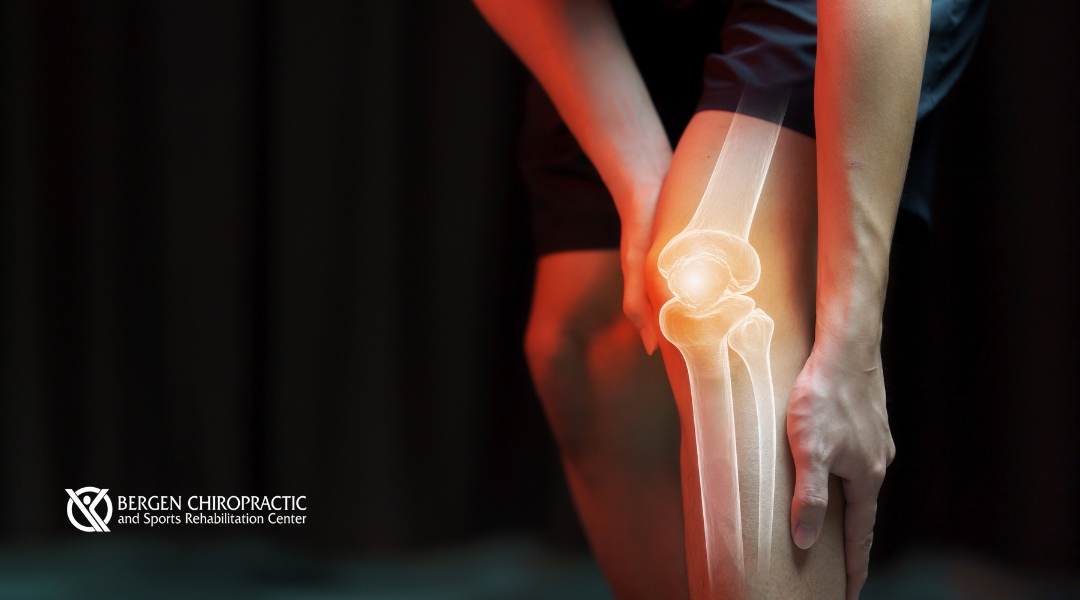
Beyond Ice Packs: How Chiropractic Care Addresses Knee Pain in Teens Holistically
Explore the benefits of chiropractic care for knee pain in teens, focusing on holistic methods for pain relief, mobility improvement, and overall wellness.